7 Breastfeeding Secrets I Wish I Knew Sooner
This post may contain affiliate links (full disclosure policy). As an Amazon Associate, I earn from qualifying purchases.
Were there things you wish someone told you about breastfeeding? Me too. I originally wrote this post in 2016 as a brand new, first-time mom. Now I’m an International Board Certified Lactation Consultant, so I’ve added some pro tips to this post. These are 7 breastfeeding secrets I wish someone told me when I was still in the hospital.
I won’t lie: I went into pregnancy with pretty low expectations of those first few days and weeks as a new mom. I knew I would be totally and completely in love with my new little bundle, that I’d adore that part of new mommyhood. But the process of actually caring for and breastfeeding a newborn sounded a little scary.

Breastfeeding getting you down?
This FREE guide will give you 12 breastfeeding secrets that will help you avoid common breastfeeding problems. Get it now for a limited time!
So I figured I would steel myself. I would assume the worst and be pleasantly surprised to find it not as hard as I told myself it would be.
New mommyhood was about 1000 times harder than I thought it would be. And most of that challenge? Was due to breastfeeding.

Breastfeeding is a learned skill. They tell you when you’re pregnant that it’s difficult, that it hurts, that it doesn’t necessarily come easy, all that good stuff. But it’s one thing to understand the idea of something being difficult, or painful, or physically and emotionally draining, and another thing to actually experience it.
But here’s the worst part: I could have avoided most of this.
If I had more breastfeeding knowledge, I could have known what to look for, and known sooner that something wasn’t right. I could have gotten help sooner.
Here’s what I wish I knew, and what they didn’t tell me in the hospital:
Medical Disclaimer: The content of this blog post is not medical advice nor is it a substitute for medical advice, diagnosis, treatment, or professional lactation care. This post is for educational and informational purposes only. It is the reader’s responsibility to review all information regarding any medical condition or treatment with a healthcare provider.
SECRET #1: BREASTFEEDING CAN BE A SURPRISINGLY EMOTIONAL EXPERIENCE
I went into pregnancy planning to breastfeed my child. And I figured if I couldn’t breastfeed for some reason, I would exclusively pump. My aunt did it and she seemed okay. She liked it, even. So if I needed to, I’d pump. No big deal. Breast milk is breast milk. It doesn’t matter how baby gets it.
And yet when it came down to it, I found my desire to breastfeed to be a surprisingly emotional thing. My baby had a terrible latch. As in, she couldn’t latch by herself at all. I was given a nipple shield in the hospital and wearing that shield was the only way I could get her to take milk from me.
The first few days my nipples were cracked and sore and bleeding. After a while though, things got better, but the nipple shield seemed to be causing problems. My baby was leaking milk everywhere, was sucking in air, and having really painful gas. And since she would only latch on the shield, I was basically a slave to it. After the 3000th time repositioning the shield and fighting to keep it on at 2am (those baby hands really like to get in the way), I was ready to toss the shield in the trash and exclusively pump.

As exasperated as I was, the thought of exclusively pumping was sort of devastating. It really shouldn’t have been, but it was. It made me feel like a failure even though I KNEW in my rational mind that couldn’t be further from the truth!
I just wanted to feed my baby the way I wanted to feed my baby, the way I was hoping to feed my baby, and not being able to do so produced emotions I wasn’t expecting.
In the end, I decided to fight for my breastfeeding relationship, even when people suggested I would be happier if I quit. And I’m glad I did.
Pushing forward was the right decision for me, and only I could make that decision. Sometimes I wondered if maybe I was “wrong” for wanting to breastfeed so badly, but I learned that there is nothing wrong with having feeding preferences. They aren’t a judgment on other parents, just a personal preference.
I also learned that breastfeeding grief is real. And it hurts. But it’s okay to feel it, and it’s nothing to be ashamed of. Sometimes it’s what motivates us to keep going. And sometimes knowing that we did everything we could gives us the peace we need to move forward.
RELATED: Healing Breastfeeding Grief
Pro-Tip from a Lactation Consultant: Needing to use a nipple shield can be a sign that baby has a latch issue that should be addressed. Nipple shields are best used under the guidance of a lactation consultant who can help you create a plan to wean from the shield and protect your milk supply in the meantime.
SECRET #2: BEWARE OF ENGORGEMENT
When my milk came in the evening of day 2/morning of day 3, I thought I was going to burst. It was like having boulders hang from my chest and it hurt. I knew it was normal to be a little engorged at first, what with the tiny size of a newborn tummy, so I thought if anything the engorgement was a good sign–more milk for baby later, right?
By the time we got home from the hospital I thought that things were getting better. The engorgement seemed not so bad. My breasts were more firm than not, but I thought that was just what milk-making breasts felt like. How was I supposed to know any different?
On the second day of being home from the hospital with baby, I found myself buried under the covers with a bad case of the chills, and a day later my OB diagnosed me with mastitis. The next 10 days were a blur of antibiotics and cabbage leaves and painful breast compressions and warm rags.
It was NOT fun. But it doesn’t have to happen to you! Keep your breasts “emptied” regularly and it shouldn’t happen at all, but if you start to feel chills or develop a fever with no other symptoms, go to your doctor right away, as mastitis can turn serious very quickly and can hurt your supply.
Pro-Tip from a Lactation Consultant: When your milk increases in volume (which can happen anytime from 2-5 days post birth) it’s normal for your breasts to feel engorged, but this is due to increased blood, lymph, and tissue swelling. If baby isn’t breastfeeding well or if you need to supplement with expressed milk, hand expression may be your best bet for getting out as much milk as possible. Additional pumping after hand expressing may be important to protect your milk supply, even if it doesn’t yield as much milk as hand expressing.
Feeling engorged at first is normal, since the body is still learning how much milk to produce. Eventually your supply will naturally regulate to meet baby’s needs. It is normal for feelings of engorgement to go away after awhile. You can learn more about what’s normal (and what’s not) in the Breastfeeding Rescue Toolbox.
SECRET #3: PUMPING MAY NOT BE INTUITIVE
I thought it would be a matter of just putting the shield on and hitting the power switch, but pumping was a little more complicated.
First of all, I didn’t have the right breast shield size and had to buy one that fits better. The trick is to have it go right around the nipple–any bigger and too much of the areola is pulled into the shield, and any smaller will result in painful pinching. Neither are effective, and you need a shield that fits correctly to be able to effectively drain your breasts and pump the most milk. I recommend getting your breast pump before baby arrives and figure out your shield size beforehand so you’re not wandering around Target engorged and half asleep (like me).
Some people’s breasts don’t respond well to a pump, but sometimes hand massaging before or during pumping can help with this. You may find that your body gets more acclimated to the pump and responds better with time and practice.
Each pump will have its own set of knobs and buttons, and sometimes you may find that different settings work better for you. For a while, I was only able to get milk out under the “letdown” setting (the setting that mimics the suckling a baby does to stimulate the initial release of milk), but after a while that changed.

Perhaps most important, don’t assume that what you pump out is what your baby takes out of you when nursing. A healthy baby with normal oral anatomy will ALWAYS remove breast milk more efficiently than a pump. You may not pump a lot of milk at first, but this does NOT mean your supply is low. The only reliable indicator that baby is getting enough is if he/she has plenty of wet and dirty diapers and is gaining weight.
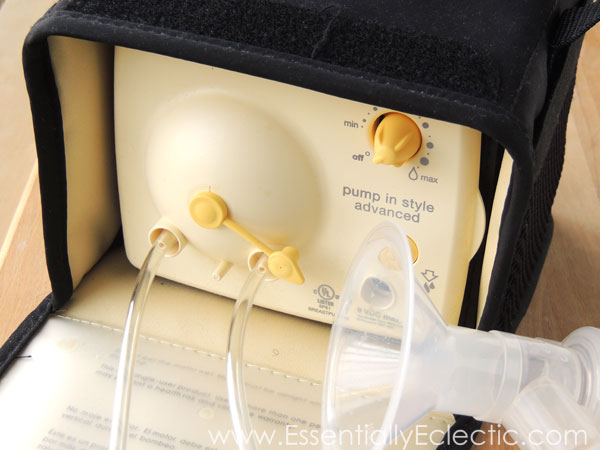
If you’re not sure what pump to buy, I highly recommend the Spectra S2 (based on the rave recommendations of friends who have used it) and the Medela Pump In Style Advanced (based on my personal experience). Medela also makes a high quality hand pump that is good to have for when you just need a few ounces of milk or to relieve the pressure of engorgement. This one–also known as the Haakaa–is also well-liked because it has only one part to wash, and you can use it to catch/draw out additional milk from the breast baby isn’t nursing on.
SECRET #4: NOT ALL IBCLCS ARE CREATED EQUAL
If you have any concerns about breastfeeding, I HIGHLY recommend seeing a lactation consultant, specifically an IBCLC or International Board Certified Lactation Consultant. And if you don’t get the answers you need or still have trouble, see a different lactation consultant.
Pro-Tip from a Lactation Consultant: The terms “lactation consultant,” “lactation counselor” and “lactation nurse” are not regulated. Anyone can call themselves one of these things. It does not necessarily mean that they are an International Board Certified Lactation Consultant. The IBCLC is considered the “gold standard” of lactation care and is the appropriate choice for both common and more complicated breastfeeding issues (e.g. tongue ties, medically fragile or premature babies, etc.) Certified Lactation Counselors or Certified Lactation Education Counselors can provide appropriate assistance and education if you are experiencing normal, uncomplicated breastfeeding issues. Nurses on the L&D floor do not necessarily have extensive lactation training.
When I was in the hospital and baby was having trouble latching on, I met with two different IBCLCs on two different occasions. Neither were what I needed. Although they were able to show me how to better position myself to breastfeed, they did not check baby for any oral abnormalities that might cause a poor latch and simply told me to hold baby against my breast more firmly.
After a couple weeks of struggling with the nipple shield at home, I decided to try my luck with a new IBCLC. I found a local center that could get me an appointment quickly and met with the most wonderful consultant I could have hoped for! She sat with me and baby for two hours, observed us feeding, offered more tips on how to encourage a good latch, how to encourage baby to suckle, and how to hold baby to best relieve gas pains.
Perhaps the most valuable thing our IBCLC did for me, however, was identify that baby had a tongue and lip tie.
SECRET #5: TONGUE AND LIP TIES ARE REAL, AND THEY AFFECT Breastfeeding MORE THAN YOU MIGHT THINK
I’d vaguely heard of ties before since one of my good friends mentioned her baby had one, but I had no idea to think to look for one or any understanding of the issues they can cause.
Many babies with ties are never diagnosed. They are often switched to bottles of formula after struggling to latch or breastfeed. Sadly, their moms are often left believing they can’t produce enough milk and feeling like they failed. Ties can be very difficult to get correctly diagnosed and are frequently missed by even experienced providers all the time. Tie symptoms are often mistaken for colic, gas, reflux, a “small mouth” or “short tongue,” and dairy sensitivity. And sometimes, they cause issues later in life, like tooth decay, sleep apnea, speech delays, and more.
Perhaps the most important thing I learned about ties, however, is that it is critical your baby is evaluated for ties by a preferred provider.
The unfortunate truth is that your average pediatrician, pediatric dentist, or ENT–although he/she may tell you he/she knows what to look for–usually does not actually know what to look for (I learned this the hard way). Some providers believe ties are a “fad,” that they don’t actually affect breastfeeding, or that they will be “fixed” with time or a fall on the face. You want a provider that understands the true significance of ties and knows how to properly correct them (simply “clipping” the tie is usually insufficient!).
You can read my full-length post on tongue and lip ties here (and you can see a complete list of preferred providers here).
SECRET #6: “LOW SUPPLY” ISN’T ALWAYS LOW SUPPLY
I’ll repeat this: the only reliable indicator that baby isn’t getting enough milk is weight gain and wet/dirty diapers. Not how much you are able to pump out, not how often baby feeds, not by how full your breasts feel, not by how much baby is crying or how hungry baby “seems,” not by how big or small your breasts are, not by how much you’re leaking or not leaking, not by any of those things.
If you are committed to breastfeeding but think you may be having issues with low supply, don’t feel like you need to automatically jump to using formula! In fact, supplementing with formula can–in some circumstances–lower a supply that wasn’t actually low to begin with. If you are concerned about supply issues, I’d encourage you to seek support from an IBCLC or reputable breastfeeding support organization like Breastfeeding USA or La Leche League.
SECRET #7: OVERSUPPLY CAN BE JUST AS PROBLEMATIC AS LOW SUPPLY
You wouldn’t think it, but it’s true. Oversupply is often associated with a fast letdown (a fast milk ejection reflex–think milk streaming from your nips and spraying baby in the face), which can cause baby to gulp and gasp while drinking. This becomes an issue later, when baby develops bad gas pains due to swallowing too much air while feeding. They say breastfed babies don’t need to burp as much, but my princess could rival a grown man with her burps!
We ended up purchasing the Rock n Play Sleeper to help, since the incline helps ease gas discomfort (UPDATE: As of 2019, the Rock n Play Sleeper has been recalled).


Oversupply can also result in lactose overload, which then causes green foamy frothy bowel movements and more acidic stool. (Don’t worry! This doesn’t mean there’s anything wrong with the milk your body is making! It’s just a sign you’re making much more than baby needs.)
If you think you have oversupply, work with a lactation consultant to diagnose the problem before taking steps to lower your supply. Your IBCLC will help you be able to rule out other issues causing your symptoms (including ties) and can help safely reduce your supply if needed so you can avoid clogged ducts and mastitis.
Breastfeeding EDUCATION IS KEY!
The best way you can prepare yourself for the breastfeeding learning curve is to educate yourself. If you’re still pregnant, now is the best time! And if you’ve already had your baby, there is still no time like the present. You can avoid stress and frustration in the future with just a little knowledge now. Learn from my mistakes.
I promise it will be worth it!

Breastfeeding getting you down?
This FREE guide will give you 12 breastfeeding secrets that will help you avoid common breastfeeding problems. Get it now for a limited time!
If you enjoyed this post, be sure to check out our digital library of helpful resources that quickly teach how to avoid common breastfeeding problems and give you the peace of mind and confidence you need to meet your breastfeeding goals.